What is cervical cancer?
Cancer is a disease in which cells in the body grow out of control. Cancer is always named for the part of the body where it starts, even if it spreads to other body parts later. When cancer starts in the cervix, it is called cervical cancer. The cervix connects the vagina (birth canal) to the upper part of the uterus. The uterus (or womb) is where a baby grows when a woman is pregnant.

All women are at risk for cervical cancer. It occurs most often in women over age 30.
What is cervical cancer?
Asthma is a condition in which your airways narrow and swell and may produce extra mucus. This can make breathing difficult and trigger coughing, a whistling sound (wheezing) when you breathe out and shortness of breath.
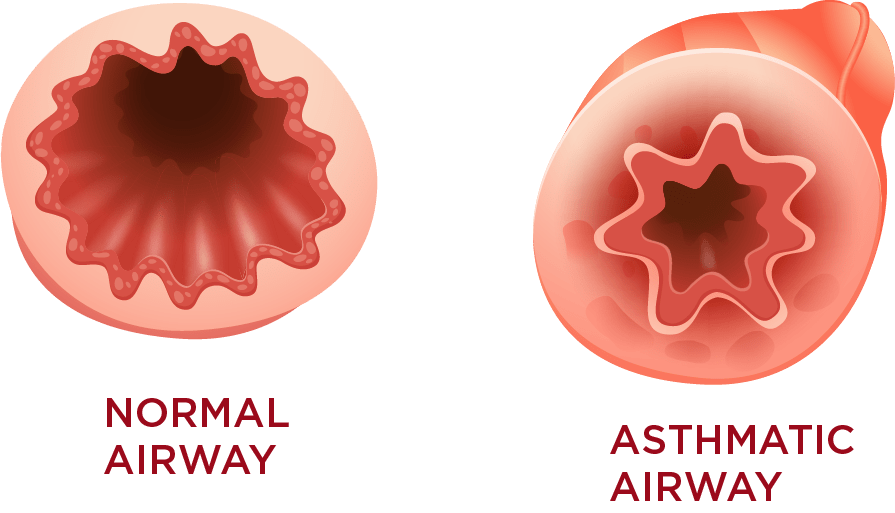

Asthma can’t be cured, but its symptoms can be controlled. Because asthma often changes over time, it’s important that you work with your doctor to track your signs and symptoms and adjust your treatment as needed.
Types of Asthma?

Allergic asthma is asthma caused by an allergic reaction. You may have trouble breathing during allergy season.

Bronchial asthma is a chronic inflammatory disease of the airways characterized by bronchial hyperreactivity and a variable degree of airway obstruction.

Nocturnal asthma is when asthma is made worse at night, associated with increases in symptoms and the need for medication.

Occupational asthma is by exposure to inhaled irritants in the workplace. It is often a reversible condition, which means the symptoms may disappear when the irritants are avoided.

Exercise-induced asthma is a narrowing of the airways in the lungs triggered by strenuous exercise. It causes shortness of breath, wheezing, coughing during or after exercise.

Steroid-resistant asthma (SRA) refers to patients with symptoms consistent with asthma who show very poor or no response at all to high doses of inhaled or even of systemic corticosteroids.
Causes
It isn’t clear why some people get asthma and others don’t, but it’s probably due to a combination of environmental and inherited (genetic) factors.
What Triggers Asthma?
Exposure to various irritants and substances that trigger allergies (allergens) can trigger signs and symptoms of asthma. Asthma triggers are different from person to person and can include:


Airborne allergens, such as pollen, dust mites.

Respiratory infections, such a common colds.

Physical Activity and Exercising.

Being in an environment with Cold Air.

Medications like Beta Blockers, Aspirin, Ibuprofen.

Strong Emotion and Strees.

Sulphites and preservatives added to some food.
Stomach acid Reflux (GERD).
Risk Factors
A number of factors are thought to increase your chances of developing asthma. They include:

Having a blood relative with asthma

Having another allergic condition like atopic dermatitis

Being Overweight

Being a Smoker

Exposure to exhaust fumes or other types of pollution

Exposure to secondhand smoke

Exposure to occupational triggers, such as chemicals

Symptoms
Most children and adults with asthma have times when their breathing becomes more difficult. Some people with severe asthma may have breathing problems most of the time. The most common symptoms of asthma are:
Wheezing
a squealing or whistling sound made when you breathe. Wheezing happens when the airways are tightened, blocked, or inflamed, making a person’s breathing sound like\ whistling or squeaking.

coughing, especially at night, when laughing, or during exercise.

Difficulty breating

A tigth chest

Difficulty Talking

Anxiousness or panic

Fatigue

Not everyone with asthma will experience these particular symptoms. If you think the symptoms you’re experiencing could be a sign of a condition such as asthma, make an appointment to see your doctor.
Asthma Diagnosis
Physical Exams
Your doctor will perform a physical exam to rule out other possible conditions, such as a respiratory infection or chronic obstructive pulmonary disease (COPD). Your doctor will also ask you questions about your signs and symptoms and about any other health problems.

Physical Exams
Tests to measure lung function. You may be given lung function tests to determine how much air moves in and out as you breathe. These tests may include:

Peak flow: A peak flow meter is a simple device that measures how hard you can breathe out.
Lower than usual peak flow readings are a sign that your lungs may not be working as well and that your Asthma may be getting worse.


Your doctor will give you instructions on how to track and deal with low peak flow readings

Spirometry: This test estimates the narrowing of your bronchial tubes by checking how much air you can exhale after a deep breath and how fast you can breathe out.
Additional Tests
You may be given lung function tests to determine how much air moves in and out as you breathe. These tests may include:

Methacholine challenge: Methacholine is a known asthma trigger. When inhaled, it will cause your airways to narrow slightly. If you react to the methacholine, you likely have Asthma. This test may be used even if your initial lung function test is normal.
Imaging tests: A chest X-ray can help identify any structural abnormalities or diseases (such as infection) that can cause or aggravate breathing problems.

Allergy testing: These tests can be performed by a skin test or blood test. They tell you if you're allergic to pets, dust, mold, or pollen. If allergy triggers are identified, your doctor may recommend allergy shots.

Nitric oxide test: This test measures the amount of gas nitric oxide in your breath. When your airways are inflamed - a sign of Asthma - you may have higher than normal nitric oxide levels.

Sputum eosinophils: This test looks for certain white blood cells (eosinophils) in the mixture of saliva and mucus (sputum) you discharge during coughing. Eosinophils are present when symptoms develop and become visible when stained with a rose-colored dye.

Provocative testing for exercise and cold-induced asthma. In these tests, your doctor measures your airway obstruction before and after you perform vigorous physical activity or take several breaths of cold air.
Treating Asthma
Treatments for asthma fall into three primary categories:

Breathing exercises
These exercises can help you get more air into and out of your lungs. Over time, this may help increase lung capacity and cut down on severe asthma symptoms. Your doctor or an occupational therapist can help you learn these breathing exercises for asthma.
Quick Acting Treatment
These medications should only be used in the event of asthma symptoms or an attack. They provide quick relief to help you breathe again. Bronchodilators work within minutes to relax the tightened muscles around your airwaves.

01
Anti-inflamatories
Taken with an inhaler, corticosteroids and other anti-inflammatory medications help reduce swelling and mucus production in your airwaves, making it easier to breathe.

Anticholinergics
Taken with an inhaler, corticosteroids and other anti-inflammatory medications help reduce swelling and mucus production in your airwaves, making it easier to breathe.
02
03
Long-acting Bronchodilators
These should only be used in combination with anti-inflammatory asthma medications.


Anticholinergics
These new, injectable medications may help people with severe asthma.
04
Lifestyle
These healthful habits can help people manage their Asthma:

Quit Smoking

Reach or maintain a moderate weight

Be physically Active

Quit Smoking

Reach or maintain a moderate weight

Be physically Active
Asthma Action Plan

Work with your doctor to create an Asthma action plan that outlines in writing when to take certain medications or when to increase or decrease the dose of your medications based on your symptoms. Also include a list of your triggers and the steps you need to take to avoid them. Your doctor may also recommend tracking your asthma symptoms or using a peak flow meter on a regular basis to monitor how well your treatment is controlling your Asthma.
Prevention
While there’s no way to prevent asthma, you and your doctor can design a step-by-step plan for living with your condition and preventing asthma attacks.

Follow your Asthma action Plan

Get vaccinated for influenza and pneumonia

Identify and avoid asthma triggers

Monitor your Breathing

Take your medication as prescribed

Pay attention to increasing quick-relief inhaler use
